Technology- based teamwork

The past few decades have seen a great improvement in surgical technology and instruments, but the future holds limitless opportunities for advancements that will lead to safer, more precise surgeries with better outcomes for patients.
Many of those improvements — both small and large — are being designed and tested at Vanderbilt University Medical Center, many due to a strong and “extraordinarily unique” collaboration between VUMC and the Vanderbilt Institute for Surgery and Engineering (VISE), said Erin Gillaspie, MD, MPH, FACS, assistant professor of Thoracic Surgery and a surgeon who has collaborated with VISE.
Gillaspie said that the leaders of VISE have taken great strides to integrate themselves into the surgical world, even moving onto the Medical Center campus to make it easier for surgeons to spend time with VISE engineers designing new ideas, creating protocols and writing proposals, and helping to test and refine new devices.
“Equally, it has allowed the teams of engineers to come spend time in the clinical setting, including the operating rooms, which has allowed them to have a deeper understanding of our current technologies, applications and hurdles that we are working to overcome,” she said.
“The partnership of engineering and surgery, to me, is one that is both extraordinarily exciting and incredibly useful,” Gillaspie said. “While we have seen a great expansion in technology and instruments, especially in the past two decades, there are still so many opportunities to both enhance current technologies as well as to develop new ones.”
Many current devices, while excellent, have significant shortcomings that have been a challenge to overcome, Gillaspie said. “For example, our standard laparoscopic tools are using cameras that only project images to us in two dimensions. And robotics have advanced tremendously but are lacking in haptic feedback – this means that the surgeons can’t feel the tissues they are working on. We are all excited to see and help design the future of surgery through further miniaturization of instruments and robots to allow us to do more and more complex surgeries through smaller incisions – ultimately leading to enhanced recovery for patients.”
A company co-founded by Robert Webster III, PhD, Richard A. Schroeder Professor of Mechanical Engineering and associate professor of Medicine and Urology at Vanderbilt University, received a breakthrough device designation from the Food and Drug Administration. The company, EndoTheia, Inc., is based on technology originally invented at Vanderbilt and the University of Tennessee. The device is based on extremely thin-walled, laser-machined metallic tubes enabling the creation of flexible, steerable devices that can pass through standard endoscopes while also carrying within themselves interventional tools.
“The team at EndoTheia, Inc. is working to revolutionize the ability to perform complex procedures via scopes through automation, enhancing precision, and the availability of platforms and tools,” said Gillaspie, a lung surgeon. “For something like lung cancer, where nodules can be difficult to reach, this allows for a highly accurate diagnosis, and as our therapeutic options continue to expand, systems like they are creating will also allow for the delivery of new treatments for patients. Perhaps most uniquely for a team like theirs is that they have partnered seamlessly with the physicians using the technology to ensure that each instrument is designed with the intuitive adoption and maximum benefit,” she said.
Gillaspie said that the field of robotics has also grown significantly over the past decade, and surgeons believe it will continue to improve current and new treatment applications for patients.
“I am looking forward to a future that will allow for the combinations of extraordinary existing technologies to provide more precise, safer surgery for patients and the continued development of newer, better technologies that will genuinely replicate the ability to do surgery in open fashion without sacrificing view, dexterity, touch or sensation.”
On the following pages are some of the new surgical devices currently being designed and tested at VUMC. – Nancy Humphrey
Expandable prosthesis

Last year Dominic Gamez was an active 7-year-old boy who loved playing travel soccer.
Then, in January, after complaining of pain in his left leg, a biopsy at Monroe Carell Jr. Children’s Hospital at Vanderbilt confirmed a diagnosis of osteosarcoma, cancer that originates in the bone-forming cells. Treatment requires a combination of chemotherapy and surgery.
“Osteosarcoma is the most common bone cancer seen in children and is highly malignant,” said Scott Borinstein, MD, PhD, professor of Pediatrics in the Division of Pediatric Hematology/Oncology at Vanderbilt University Medical Center and director of the Pediatric Sarcoma Program at Monroe Carell. “Eighty percent of all osteosarcomas occur around the knee, like Dominic’s did,” he said.
Dominic had an 8-inch tumor involving two-thirds of his femur, extending from the bottom of the femur near the growth plate (at his knee) to the femur shaft. Growth plates are the biologic machines that make new bone so that we can grow. In addition to removing the cancerous bone, necessary for a cure, often surgery to remove osteosarcoma involves the removal of growth plates, so there are anticipated growth discrepancies, too.
His family was given three choices: amputate; replace the resected femur with a cadaver bone (allograft); or implant a magnetic expandable prosthesis that can be manipulated to grow incrementally as the child grows.
The family chose the magnetic expandable prosthesis for Dominic, which has been used 17 times at Monroe Carell over the past decade. It requires one surgery to remove the tumor, check the tumor’s margins and insert the implant.
“Of all the options, this gives him the best chance to be active, to be Dominic,” said Dominic’s surgeon, Jennifer Halpern, MD, assistant professor of Orthopaedic Surgery. “The expandable femur replacement/knee replacement is durable, reliable, and it grows with the child.”
For patients who choose the magnetic expandable prosthesis, advanced imaging helps to plan and build their custom implants. MRI scans help to determine the size of the tumor that needs to be removed. CT scans are used to build custom implants that match the patient’s anatomy. The size of the implant also impacts the growth potential of the device. The larger the replacement, the more the implant can be “grown.”
The surgeon writes a prescription for the implant, and it is custom built during the weeks the patient is receiving chemotherapy, pending the surgeon’s approval during the construction process.
Halpern said the magnetic expandable prosthesis is ideal for Dominic because his femur would normally grow more than 4.4 inches over the next eight years. “The combination of a durable implant that allows for weight bearing, with an option for noninvasive periodic expansion, is a powerful tool in limb salvage surgery,” she said.
After the skin has healed following the surgery, the prosthesis can be lengthened 4 millimeters at a time in the clinic with a special magnetic device that is shipped to Monroe Carell.
It takes about four minutes per millimeter and is painless. “Most patients sit and read a book or look at their phone while the lengthening process occurs,” Halpern said.
Each patient will have a schedule for monitoring leg length and lengthening — generally at six weeks after the surgery and then in three-month intervals.
Dominic, now 8, is doing well and is adjusting to the fact that it’s not recommended that he play competitive soccer or other high-impact cutting and pivoting sports. Low-impact activities like golf or swimming are ideal.
“Across the board, we don’t recommend extensive running in a prosthesis of this length, but we typically allow kids to do and try as much as they can,” Halpern said. “We want Dominic to be active, but we also want to minimize the trauma of having major surgeries that can become limb threatening,” she said.
“Kids who have an allograft can’t bear weight for months, and they can’t do a lot of athletic things because their knee joints are unstable. Dominic really hasn’t lost a step. He’s asking to do more and more, and we’ll let him do more and more as we assess if it’s safe. He’s doing a lot, and I’m grateful for that. It’s not easy to reinvent yourself, but I think he’ll be and do something miraculous,” Halpern said. – Nancy Humphrey
Monitoring heart failure patients from home

When it became impossible to keep Tony Conaway’s heart failure in balance at home, he became a candidate for a new investigational device called the Cordella System, which monitors not only his heart pressures but also his weight, heart rate, blood pressure and oxygen levels. In the spring, Conaway became the first patient at Vanderbilt to receive this new implant.
Implantable devices such as Cordella offer peace of mind to heart failure patients such as Conaway, who lives more than two hours away from Vanderbilt.
The technology allows him to have fewer in-person appointments at Vanderbilt Heart and Vascular Institute for tests and procedures and lets his team of doctors know what is going on with his heart.
“It’s enabled them to take better care of me and saves me from having to come so often from a long way away,” Conaway said.
In March Vanderbilt Heart celebrated having helped more than 100 heart failure patients with such implantable devices through its Ambulatory Heart Failure Devices Program.
“The success of the Ambulatory Heart Failure Devices Program is a great example of what Vanderbilt does best — innovation and collaboration at multiple levels to improve patient outcomes,” said Kelly Schlendorf, MD, associate professor of Medicine and section head of Heart Failure and Transplantation.
Conaway was also the 500th person to get the Cordella System in a clinical trial in which Vanderbilt Heart participated. The minimally invasive procedure to implant the device takes an average of 45-60 minutes, and patients are discharged the same day and can start using the device immediately.
Every morning, Conaway uses a handheld tablet that receives signals from the device. The tablet sends the data to his physicians.
Lynne Stevenson, MD, professor of Medicine and director of the Cardiomyopathy program at VUMC, has been taking care of Conaway for the past two years, but has been working for more than 25 years to help apply remote hemodynamic monitoring to help manage heart failure between clinic visits.
“This technology opens a window to guide what we are doing,” Stevenson said. “It has been said that the ambulatory pulmonary pressures help understand heart failure the way the electrocardiogram has helped to diagnose cardiac rhythms.”
Those who benefit from remote heart failure monitoring include patients suffering from heart failure with reduced ejection fraction, heart failure with preserved ejection fraction, congenital heart diseases, infiltrative heart diseases, pulmonary hypertension and those living with left ventricular assist devices and heart transplantation. – Matt Batcheldor
Outpatient lumbar fusion

Raymond Gardocki, MD, associate professor of Orthopaedic Surgery, played an instrumental role in developing and implanting the Flarehawk 9 — a first-of-its-kind interbody implant that can be placed endoscopically during spinal lumbar fusion surgery.
The patient Gardocki cared for had previously undergone a traditional open fusion — using a bone graft to join two vertebrae into one long bone — eight years ago. This time, due to the new device’s ultra-minimally invasive nature, she was able to recover and return to her normal activities much sooner than her previous experience with open surgery. The lumbar fusion performed by Gardocki was done on an outpatient basis without an inpatient hospital stay.
“The Flarehawk 9 is an expandable cage, but unlike some that only expand on height upon insertion, this one can expand in both height and width,” Gardocki said. “You can use a smaller corridor with less nerve retraction to place it.”
Gardocki’s extensive experience in endoscopic surgery meant he was well equipped to help develop the instruments for endoscopic insertion of the new device when he was asked to join the effort to develop it.
Gardocki built the preliminary endoscopic insertion cannula, which can now be inserted through a 13-millimeter diameter before expanding to 14 millimeters tall and 14 millimeters wide. For perspective, a dime measures 18.5 millimeters in diameter.
Gardocki is also able to perform the implantations on patients under conscious sedation without the need for intubation — often on elderly patients who may not be able to tolerate general anesthesia.
Since the new implant can expand farther than previous iterations, it is particularly useful for large-framed people who need to undergo spinal lumbar fusion. For people of larger stature, previous implants were often too small for optimal support.
“I compare this work to building a ship in a bottle,” Gardocki said. “It’s become so minimally invasive that I’m now able to do these as an outpatient procedure.”
One of the most common conditions Gardocki treats with endoscopic interbody implants is degenerative spondylolisthesis. – Emily Stembridge
Implantable Bilateral Pacemaker for Vocal Paralysis
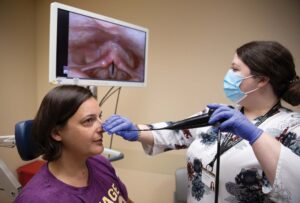
Injury to both vocal cords (bilateral paralysis) is common in cancer patients who have had a resection and makes patients feel like they are being strangulated.
Persons with this condition have vocal folds frozen in the near-closed position, which can make it difficult to breathe, according to David Zealear, PhD, professor of Otolaryngology – Head and Neck Surgery at VUMC.
“The standard of care for these patients has been to enlarge the airway to improve breathing, but this sacrifices the patient’s ability to speak,” Zealear said.
Zealear led a first-of-its-kind laryngeal pacer clinical trial at VUMC.
In fact, Vanderbilt is the only place in the world that has an implantable bilateral pacemaker that can stimulate opening of both vocal folds in patients with bilateral vocal fold paralysis, allowing them to both breathe and speak.
Further, the opening is much larger than that achieved by surgical enlargement, providing the patient with the capacity to engage in strenuous exercise.
After decades of researching possibilities for reanimation of a paralyzed muscle, Judit Kiss, 40, who lives about 25 minutes outside of Denver, was the first patient in the National Institutes of Health-funded clinical trial.
“She was the perfect candidate, and I could not have hoped for a better result — this is a really amazing proof of concept,” Zealear said.
There are 7,000 new patients each year diagnosed with vocal paralysis and a total of more than 80,000 patients living with the condition across the world who would be candidates for the surgery, he said. His clinical trial is enrolling eight patients, with hopes to expand to multisite studies moving forward.
Kiss has a pacer implanted under her skin that cycles on for three seconds and off for three seconds, synced with her breathing rate, to allow her vocal cords to open.
“This allows me to do everything. I am not kidding when I say I have not been able to work out for six years,” she said. “I have always been an athlete; I have always been active, so it was really frustrating to not be able to do that.
“Now my pacer is implanted, and it is on, and it is cranking. I recently was able to dance at my best friend’s wedding, and there is no way I could have done that before. And I don’t feel it, it just does its thing,” she said.
Eben Rosenthal, MD, Odess Professor of Otolaryngology- Head and Neck Surgery and chair of the department, classifies the operation both as a success in itself and as necessary preparation for laryngeal transplants.
“Dave has been able to give new breath — pun intended — into new patients,” Rosenthal said.
“Every day not being able to breathe as you go up a flight of stairs or walk any kind of distance is just incredibly traumatic, and it is a feeling of asphyxiation. It is like being smothered.”
Perhaps what is most exciting is the opportunity for using this idea in other settings, Rosenthal said.
“Many people get their voice boxes taken out for cancer, and we could conceivably transplant them if we had a way to open the vocal cords.
“The implications of this are not just for an unusual disease but for a common disease like throat cancer where you could conceivably give them a transplant with moving vocal cords.” – Craig Boerner
Neuromodular Stimulation
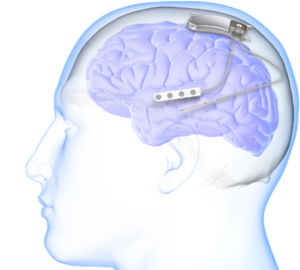 A female adult patient with idiopathic generalized epilepsy (IGE) was the first to receive neuromodular stimulation of the brain to see if it can help with seizures.
A female adult patient with idiopathic generalized epilepsy (IGE) was the first to receive neuromodular stimulation of the brain to see if it can help with seizures.
IGE, which is diagnosed in childhood or adolescence and often results in lifelong seizures, accounts for 15-30% of epilepsies.
It is the second most common type of epilepsy, after focal onset epilepsy, but there are currently no FDA-approved devices available, according to VUMC co-investigator Angela Crudele, MD, assistant professor of Neurology.
“We have limited treatment options for patients who have drug-resistant, idiopathic generalized epilepsy,” she said. “I am excited about the possibility of having an FDA-approved treatment for this population, such as a brain-responsive neuromodulation, and giving these patients a better future.”
The NAUTILUS clinical study is evaluating safety and effectiveness of the RNS System in individuals age 12 and older with drug-resistant IGE, also known as primary generalized epilepsy. The first procedure took place at VUMC with Crudele and co-investigator Dario Englot, MD, PhD, associate professor of Neurological Surgery.
The RNS System is the only FDA-approved brain-responsive neuromodulation system that delivers personalized, targeted treatment at the seizure source. Its closed-loop technology monitors and responds to a patient’s unique brain patterns to deliver therapy in real time, typically before clinical symptoms occur. – Craig Boerner
Promising possibility for pancreatic cancer

Maudean Armour of Clarksville, Tennessee, was the first patient in Tennessee to undergo intraoperative radiotherapy for pancreatic cancer, a new technology that targets any remaining cancer cells with electrons during surgery.
The IntraOp Mobetron IORT with electrons at Vanderbilt University Medical Center makes surgery possible for patients with pancreatic cancer who may have been told their tumors are inoperable because of involvement of major blood vessels.
Armour had been told her tumor was inoperable because of its proximity to major blood vessels, including the aorta. The procedure was performed by surgical oncologist Kamran Idrees, MD, MSCI, MMHC, Ingram Associate Professor of Cancer Research, and radiation oncologist Natalie Lockney, MD, assistant professor of Radiation Oncology.
Vanderbilt, the only Center of Excellence for pancreatic cancer in Tennessee as designated by the National Pancreas Foundation, is also the only hospital in the state with this advanced surgical technology. Idrees specializes in treating complex cancers of the pancreas, liver and bile ducts that may involve major blood vessels and adjacent organs. His patients include people with pancreatic and other abdominal cancers who have been told their tumors are inoperable.
“We are encouraged by the results of treating localized pancreatic cancer with electrons during surgery,” said Idrees, chief of the Division of Surgical Oncology and Endocrine Surgery. “We serve our patients by implementing the latest innovations at Vanderbilt to improve outcomes.”
Pancreatic cancer remains one of the deadliest forms of cancer. The location of the pancreas with its proximity to major vessels, duodenum, stomach, small and large bowel, liver and kidneys makes precision critical.
“With the precision of intraoperative radiation therapy, we can target any remaining cancer cells on or near blood vessels to vital organs to preserve them. With this technology, we can precisely give radiation to the area of concern during surgery while avoiding radiation to other organs,” Idrees said.
IORT with electrons makes precise surgery available for more patients than ever before, IntraOp Medical Corporation said in a press release.
“While this procedure is a first for the extraordinary team at Vanderbilt University Medical Center, it is yet another chapter for the promise of IORT with electrons and our collective fight to better treat pancreatic cancer,” said Sanjay Arora, CEO at IntraOp. “We’re excited to see where this important milestone leads us.”
The Vanderbilt Pancreas Center offers a protocol that prioritizes time to treatment, second opinion sessions, a multidisciplinary clinic and a nurse navigator to personally assist patients. – Tom Wilemon
