Training and Requirements
Mentor Selection
To facilitate the seamless integration of the research and clinical aspects of the program each student has an assigned Basic Science Mentor as well as a Clinical Mentor. These two mentors guide students in their choice of didactic courses, clinical seminars and clinician interactions.
Basic Science Mentors: All participating graduate students have already identified their thesis mentor when they matriculate in the program. The thesis adviser also serves as the Basic Science Mentor for the APMM. Similarly, the research mentor for postdoctoral trainees also serves as the Basic Science Mentor for the APMM. All full-time basic science tenured and tenure-track faculty members at VUMC are eligible to serve as Basic Science Mentors.
Clinical Mentors: The selection of the Clinical Mentor for each incoming participant is paramount for the success of this program component. The trainee, in consultation with his/her Basic Science Mentor suggests three Clinical Mentors for consideration at the time of application to the APMM. The Advisory Committee reviews this list and assigns a Clinical Mentor for successful applicants. The clinical mentor is encouraged to participate in thesis or advisory committee meetings during the course of the program, but is not required to be a standing member.
Training Requirements
Training requirements for the program consist of the following four major components, all designed to provide a solid grounding in how modern biomedical research impacts a range of disease states:
- Clinical Contact Hours
- Didactic Course Work
- Seminars and Bench-to-Bedside Symposia
- Annual retreat
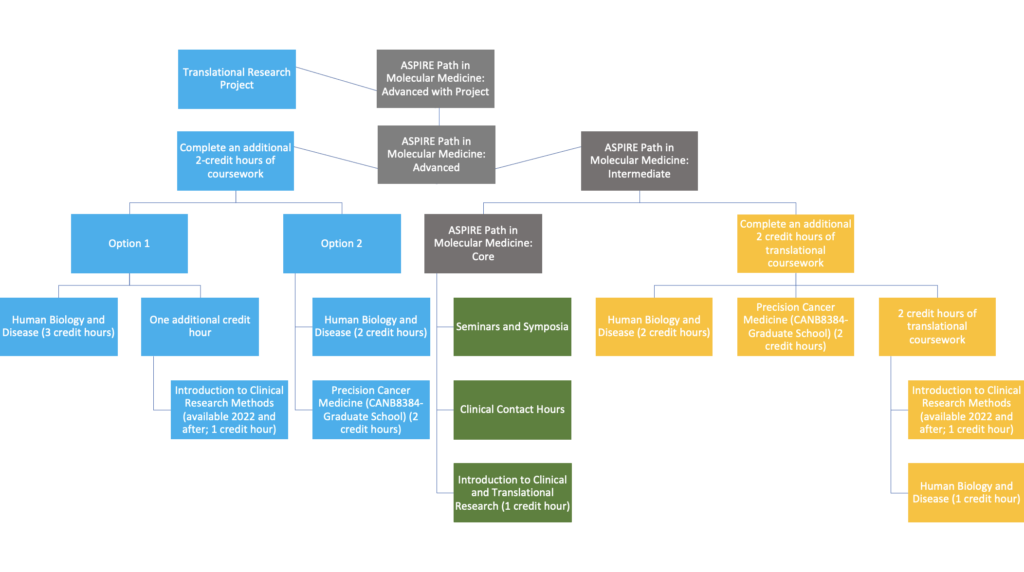
Students can elect to take CORE, Intermediate, Advanced, or Advanced PLUS with a Clinical Project APMM curriculum tracks, over 2 or 3 years, depending on which track they select.
- CORE APMM track students will complete the required clinical contact hours and attend the required number of seminars and bench to bedside symposia, and attend “Introduction to Clinical and Translational Research” for audit or credit (1 hour/spring semester). This should be completed in two years
- Intermediate APMM track students will meet the requirements for CORE APMM track PLUS attend an additional two credit hours of didactic course work provided for APMM students for audit or credit. This should be completed in two years
- Advanced APMM track students will meet the requirements for CORE APMM track PLUS attend an additional four credit hours of didactic course work provided for APMM students for audit or credit. This should be completed in two years
- Advanced APMM with a Clinical Project track students will meet the requirements for Advanced APMM track PLUS complete a clinical research project which they will present at one of the APMM seminars or annual retreats. This may be completed in up to three years. Note students completing over three years will be required to continue attending seminars and bench to bedside symposia in their third year as well.
Major training components
Clinical Contact Hours:
We have created 3 different opportunities for clinical exposure. Students are expected to accumulate a total of 30 hours comprised of any combination of these activities over the course of the 2- or 3-year program. These include:
- Physician-Patient Interactions in clinical settings [up to 20 hours]. Each student will be assigned a clinical mentor who they will meet early in the program to discuss their interests and opportunities for clinical exposure in different clinical settings at VUMC.
- Clinical Case Conference [up to 10 hours]. These are clinical management and/or clinical diagnosis case conferences that are typically given by medical residents and fellows in individual specialty departments at VUMC. Students will be able to find out about these from their clinical mentor.
- Simulated Patient Interviews[up to 6 contact hours]. The Center for Experiential Learning and Assessment (CELA) at Vanderbilt provides students with the opportunity to interview trained actors who simulate clinical conditions that commonly occur in practice. This provides APMM students with the unique opportunity to experience the process of clinical assessment and evaluation of patients. After each interview students undergo a feedback session with faculty mentors who will go over their clinical finding, differential diagnosis, and management plans for a patient with this condition. Please sign up in advance for one or more of these clinical opportunities from 9:30am till noon on December 14th, 2023, Feb 15th and April 18th, 2024. Each session will have two different clinical cases. You can attend as an observer, interviewer, or both. Instructions on how to conduct a clinical interview are included in this sign-up form.
- NIH Demystifying Medicine Series[up to 5 contact hours]. This seminar series is jointly sponsored by FAES and NIH, and includes presentations on pathology, diagnosis, and therapy in the context of major disease problems and current research. Primarily directed toward PhD students, clinicians and program managers, this series is designed to help bridge the gap between advances in biology and their application to major human diseases. Each session includes clinical and basic science components presented by NIH staff and invitees. You can attend seminars in real time or watch recorded videos and enter the activity under clinical contact hours in the APMM course management system. For more information and details about the seminar series, visit the website: https://demystifyingmedicine.od.nih.gov/
Didactic Courses: This component of the APMM is divided into specific units, usually relating to a specific pathobiology. Most units are a mix of formal presentations as well as opportunities to observe patients or to examine pathologic material. These units vary from semester to semester, are highly flexible and can be custom designed by the trainee, in consultation with the joint mentors, to suit individual requirements, and their selected APMM track (see below). These are:
- Introduction to Clinical and Translational Research (1 credit hour): This is a spring semester IGP module that has been designed to provide a broad introduction to the principals and challenges of human subjects research today. Topics covered include clinical trials, drug development and regulation, biorepositories and EMR, IRB and ethical considerations, and translational research support and opportunities at Vanderbilt. This is the only required course for all students participating in APMM (for credit or audit)
- Introduction to Clinical Research Methods (1 credit hour): This course uses didactic and case-based approaches to demonstrate practical tools to facilitate translational research. There will be 12 topics taught each over one-hour blocks coordinated by a basic scientist or physician scientist with experience in translational research. The last session will conclude with student proposals to incorporate a clinical or translational component into their research program using methods discussed in the course. For students selecting the Advanced APMM track with a Clinical Research Project, course directors will facilitate connections between the student and clinical researchers at VUMC if this is required to help them develop a clinical research project.
- Human Biology and Disease (1-3 credit hours): The aim of this course is to provide students with a comprehensive, organ-based overview, of human biology and disease pathophysiology from a clinical perspective. There will be 15 disease topics taught over a three-week period, each over 2-hour blocks coordinated by a physician or physician scientist involved in treating patients with common diseases affecting different organ systems. Most units are a mix of formal presentations as well as opportunities to interact with patients with the disease being discussed at that session. Students will be able to preselect to attend all 15 sessions for 3 credit hours, or, based on their interests, select 10 sessions for 2 credit hours, or 5 sessions for 1 credit hour. If they select only to attend 5 or 10 sessions, they will be able to preselect which disease topics they attend.
Seminar Series and Bench-to-Bedsides Symposia
To meet the requirements, attendance of 70% must be met for the Seminar Series and Bench-to-Beside Series each year while trainees participate in the APMM (i.e.: for 2- or 3-years, depending on the APMM track they select).
- Program Orientation: All new trainees attend three weekly orientation meetings in September. These meetings are held to ensure that all new members in the program understand all the component parts and their role over the next 2-3 years.
- Seminar Series: The seminar series meeting is a forum for all participants to discuss progress in the program or to bring up any issues that may have arisen. This is followed either by a research presentation by a trainee, or by an invited speaker. These are typically held on the third Wednesday of the month from 5:00 pm – 6:00 pm in Light Hall 306.
- Bench-to-Bedside Symposium: The APMM has developed the “Bench to Bedside” mini-symposium series as a forum to enhance interaction and discussion between the various Vanderbilt graduate and post-doctoral education programs and clinical scientists involved in patient care. The format and topics vary at each meeting but in principal focus around both clinical and research related to a particular disease. Presenting faculty are often accompanied by a patient to expose trainees to the social and personal impact the particular disease and its treatments can have on individual patients. These sessions are typically held on the first Wednesday of the month from 5:00 pm – 6:00 pm in Light Hall 419.
Annual Retreat
The APMM organizes a one-day annual retreat, usually early June, which alternates between on site and off site every other year. Trainees are expected to attend the retreat each year they participate in the APMM (i.e.: 2 or 3 annual retreats, depending on the APMM track they select)
Program Tracks and Timeline
Students can elect to take CORE, Intermediate, or Advanced APMM curriculum tracks, over 2 or 3 years, depending on which track they select.
For more information on APMM tracks, learn more on the Badgr platform. The ASPIRE Path in Molecular Medicine: Advanced Badge awarded to learners who complete the three core components of the APMM program (including the 1-credit hour course, “Introduction to Clinical and Translational Research”) plus an additional four credit hours of courses and a translational research project. Learners may complete credit hours either by registering for-credit or by auditing the course.